Blogs
Downregulation and Upregulation of Receptors
Ruth Fisher
In a previous blog entry, Overview of How the Endocannabinoid System Works, we described how our Endocannabinoid Systems (ECSs) contain three basic sets of components:
- Cannabinoid receptors: Receptors on cell membranes that are activated by cannabinoids
- Cannabinoids: The messengers, or neurotransmitters, that activate cannabinoid receptors
- Cannabinoid enzymes: The enzymes that break down, or inactivate, cannabinoids
Each type of cell has a particular speed at which new cell receptors are naturally synthesized and then subsequently degraded. However, activation of cell receptors by messengers causes receptors to degrade more quickly.[1]
The number of receptors present on the cell at any given time thus depends on how quickly new receptors are being synthesized, relative to how quickly existing receptors are degrading. If receptors are degrading faster than they’re being synthesized, then the total number of receptors on the cell will decrease, or experience downregulation. Conversely, if receptors are being synthesized faster than they’re degrading, the total number of receptors on the cell will increase, or experience upregulation (see Figure 1).
Figure 1: Upregulation and Downregulation of Cell Receptors
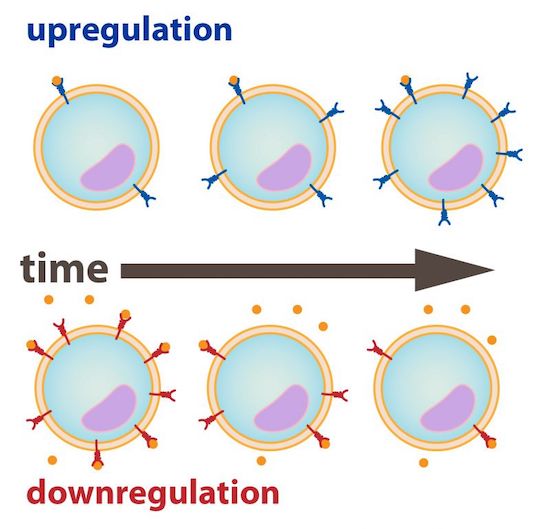
Source: Downregulation and upregulation. (2019, Feb 19). Retrieved from https://www.turkaramamotoru.com
The level of endocannabinoid activity in an area of your body – which includes the extent of upregulation or downregulation of cannabinoid receptors – is called endocannabinoid tone.
New messengers introduced into your system – either through natural production or through ingestion (say, by taking medication) – will have a greater impact when more cell receptors are present. That is, your body will be more sensitive to the messengers. Conversely, new messengers will have a smaller impact when you have fewer receptors.
Generally, we’ll take a new medication because our bodies are not producing enough of the chemical on its own. We’re suffering from a shortage of supply. In this case, we tend to be more sensitive – that is, have more cell receptors available. Smaller doses will then have a greater effect.
However, if we’ve been taking a medication regularly, our bodies will become desensitized – that is, the number of receptors will be downregulated. In this alternative case, then, we need a stronger dose to generate the same effect we used to get from a smaller dose.
Take a specific example: our ECS has been shown to modulate pain and inflammation. We know this because scientists have examined animals and people who are experiencing pain and inflammation. In the bodies of those suffering from pain and inflammation, scientists find upregulated numbers of cannabinoid receptors.[2] In other words, pain and inflammation are being caused by not having enough cannabinoids in your system. Cannabis thus helps relieve pain and inflammation by addressing your bodies’ needs for more cannabinoids.
As another example of how upregulation of our ECS accompanies diseases in our bodies, in The Endocannabinoid System: A Beginner’s Guide, the Leaf Science Editorial Team notes:
Besides maintaining basic functions, the endocannabinoid system also acts in response to illness.
For example, tumor cells have been shown to express more cannabinoid receptors than healthy cells. Studies also show a rise in endocannabinoid levels in patients with various disorders, such as Parkinson’s disease, anxiety, chronic pain and arthritis.
Sources:
[1] McIntosh, H., Song, C., and Howlett, A. (1997, Sep 2). CB1 cannabinoid receptor: cellular regulation and distribution in N18TG2 neuroblastoma cells. Molecular Brain Research. Retrieved from https://www.researchgate.net/publication/13756565_CB1_cannabinoid_receptor_Cellular_regulation_and_distribution_in_N18TG2_neuroblastoma_cells
[2] Manzanares, J. and Carrascosa, A. (2006 Jul). Role of the Cannabinoid System in Pain Control and Therapeutic Implications for the Management of Acute and Chronic Pain Episodes. Curr Neuropharmacol. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2430692/

