Throughout history, bacterial infections have been the scourge of human beings. Up until the early 1900s, the top 10 leading causes of death globally were all bacterial infections, most of them infectious diseases. Between the late 1800s and early 1900s, however, the introduction of public sanitation measures, together with the advent of vaccines, significantly curtailed death from bacterial infections, particularly in more developed nations. Nonetheless, while sanitation and vaccinations prevent much bacterial infection from occurring, they certainly do not eliminate all infections, nor do they treat the infections that do occur.
In a previous blog entry, Overview of How the Endocannabinoid System Works, we described how our Endocannabinoid Systems (ECSs) contain three basic sets of components:
- Cannabinoid receptors: Receptors on cell membranes that are activated by cannabinoids
- Cannabinoids: The messengers, or neurotransmitters, that activate cannabinoid receptors
- Cannabinoid enzymes: The enzymes that break down, or inactivate, cannabinoids
Each type of cell has a particular speed at which new cell receptors are naturally synthesized and then subsequently degraded. However, activation of cell receptors by messengers causes receptors to degrade more quickly.[1]
The number of receptors present on the cell at any given time thus depends on how quickly new receptors are being synthesized, relative to how quickly existing receptors are degrading. If receptors are degrading faster than they’re being synthesized, then the total number of receptors on the cell will decrease, or experience downregulation. Conversely, if receptors are being synthesized faster than they’re degrading, the total number of receptors on the cell will increase, or experience upregulation (see Figure 1).
I’m a researcher. Just over two years ago, I was introduced to the subject of medical cannabis. My quest was to understand how cannabis works in our bodies to provide medicinal benefits. It’s been a little over two years since I started my research, and I’ve learned quite a bit.
The more I’ve read, the more overwhelmed I’ve become at how extraordinarily complex the human body is. Our bodies are the product of millions of years of evolution, and it shows. Our bodies are like tremendous orchestras, with more instruments in our bodies (cells) than there are stars in the sky. And not only are there brass and string and percussion instruments – akin to our circulatory and digestive and immune systems – but within each system there are scores of sub-systems. Within the wind instruments are numerous flutes and oboes and clarinets and saxophones and bassoons.
The average human body contains about 33 trillion cells of about 200 different types, 100,000 miles of blood vessels, and 640 skeletal muscles. Every day, the average adult takes over 20,000 breaths, experiences 100,000 heartbeats, processes about 200 quarts (50 gallons) of blood through the kidneys, and filters out about 2 quarts of waste and water.
So how does the Endocannabinoid System (ECS) in our bodies work? To understand this, we first have to understand some basics about cells and cell-to-cell communications.
Cells
A cell is the smallest unit of life. Cells are often called the "building blocks of life." Our bodies are comprised of trillions and trillions of different cells, approximately 32.7 trillion cells in all, of more than 200 different types.
Cells Cluster
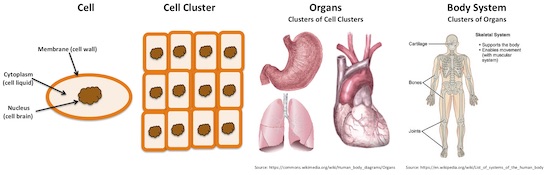
Each cell has a particular function to perform. At the same time, however, cells cluster to form tissues, organs, and body systems, where they work together with other cells to serve larger functions (see Figure 1)
Figure 1: Cell Clusters
Benefits of Whole Plant Medicine
My brother has multiple sclerosis (MS). MS is a degenerative disease affecting the brain and spinal cord; it generally causes problems with vision, balance, and muscle control.


